
Additionally, the reporting provides an understanding of how patients receive care for common, acute and chronic conditions. The knowledge gained can positively impact resources and outreach strategies.
Identifying gaps in care is a difficult task, because in New York, patients often receive care across multiple healthcare provider networks. This presents a challenge in identifying tests and procedures that may have already been performed elsewhere.
The Gaps in Care report is a new Healthix solution that delivers data for specific HEDIS quality metrics to facilitate Healthix customers in identifying patients whose care gaps have been closed elsewhere.
The primary audience of this report is Healthix participants who focus on care coordination and quality improvement to optimize their fee schedules under various value-based reimbursement models. This report enables customers to reduce care coordination expenses and increase VBC premiums and bonuses.
Healthix uses the HEDIS Measure specifications and the HEDIS Value Set Directory to search for matches to diagnosis codes, procedure codes, lab codes and more. It then gathers the data for all consented patients at the receiving facility who have a code match and compiles it into a single report for each measure.
The Healthix consolidated Gaps in Care report contains the following measures and individual lookback period, organized in separate tabs in a downloadable file:
| MEASURES | LOOKBACK PERIOD |
|---|---|
| Adherence to antipsychotic medication (SAA) | 1-year lookback |
| Asthma medication ratio (AMR) | 1-year lookback |
| Annual visits | 1-year lookback |
| Controlling blood pressure (CBP) | Current measurement, 1-year lookback |
| Breast cancer screening (BCS) | 2-year lookback |
| Cervical cancer screening (CCS) | 5-year lookback |
| Colorectal cancer screening (COL) | 10-year lookback |
| Comprehensive diabetes care (CDC) | 1-year lookback |
| Follow up after emergency department visit for alcohol and other drug abuse or dependence (FUA) | Current measurement (30 and 7-day period) |
| Follow up after emergency department visit for mental Illness (FUM) | Current measurement (30 and 7-day period) |
| Viral suppression load | 1-year lookback |
*HEDIS (Healthcare Effectiveness Data and Information Set), QARR (Quality Assurance Reporting Requirements)
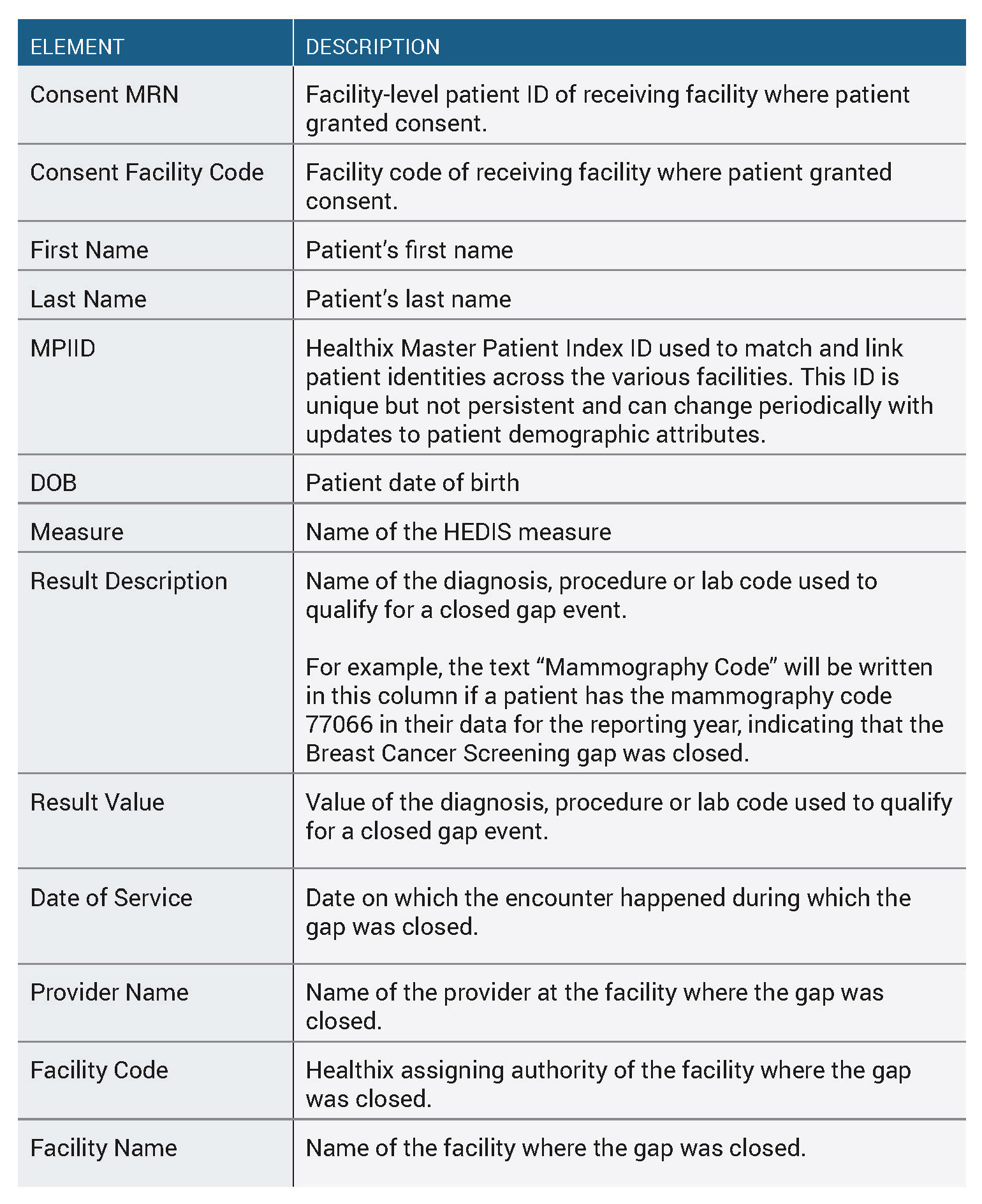
Currently the report includes the following fields:
![]()
Providing insight to help manage population health, research, high risk patients, outreach resources and more.

For health systems and clinicians, one of the most effective actions taken by Healthix might have been an effort that began before the start of the pandemic: Healthix Gaps in Care. The new service empowers healthcare organizations to identify and analyze discrepancies between best practices and actual healthcare services delivered, zeroing in on Healthcare Effectiveness Data and Information Set (HEDIS) gaps in care. Through the pandemic and into the future, the service supports Healthix participants with the data-driven insights necessary to improve quality measures and patient outcomes.
— InterSystems